
Frequently Asked Questions (Work in Progress)
What causes Tuberous Sclerosis Complex (TSC)?
Tuberous sclerosis complex is a genetic disease. A change (mutation/pathogenic varient) in the TSC1 or TSC2 gene, which normally suppress cell growth, leads to abnormal tissue and tumor growth causing Tuberous Sclerosis Complex (TSC). Only one of the genes needs to be affected for TSC to be present. The TSC1 gene is located on chromosome 9 and is called the hamartin gene. The other gene, TSC2, is located on chromosome 16 and is called the tuberin gene. TSC is autosomal dominant which means it is not linked to the sex genes and males and females have an equal risk of having the condition.
It can be inherited from one parent with TSC or can result from a spontaneous genetic mutation. About one-third of people with TSC inherited the genetic condition from a parent. However, for the other two-thirds, the condition is "spontaneous," meaning that the change is the first time of that change in the child's family. A parent with tuberous sclerosis has a 50 percent chance of passing the condition to their children.
Sometimes it is found that a child with TSC has a parent who also has the condition but didn’t know they had it. If your child is diagnosed with TSC, you may want to check that you dont also have it.
If you have one child with TSC, there is an increased chance that your other children will also have the condition.
More informatio about the genetics of TSChttps://www.tscalliance.org/understanding-tsc/genetics/
More information on autosomal dominant inheritancehttps://www.genomicseducation.hee.nhs.uk/genotes/knowledge-hub/autosomal-dominant-inheritance/
How common is TSC?
TSC affects approximately 1: 6,000 to 1: 10,000 live births. It is estimated there are between 1-2 million people in the world living with TSC. Many cases may remain undiagnosed for years or decades due to the relative obscurity of the disease and the mild form symptoms may take in some people.
What is the treatment and is there a cure?
There is no cure, but symptoms are managed with medications (like mTOR inhibitors for tumors), therapies (physical, occupational, speech), and sometimes surgery for tumors or severe epilepsy. There are international clinical consensus guidelines for the dignosis, surveillance and management of the symptoms. (See section on Diagnosis & Management)
What is the prognosis?
TSC varies widely from affecting people mildly to very severely and symptoms change over time; many live full lives with a normal lifespan, though some can face severe challenges. There can be complications in some organs such as the kidneys and brain that can lead to severe difficulties and even death. To reduce these dangers, people with TSC should be monitored throughout their life by their physician for potential complications. Thanks to research findings and improved medical therapies, people with tuberous sclerosis complex are experiencing better health care than before. https://www.ninds.nih.gov/health-information/disorders/tuberous-sclerosis-complex
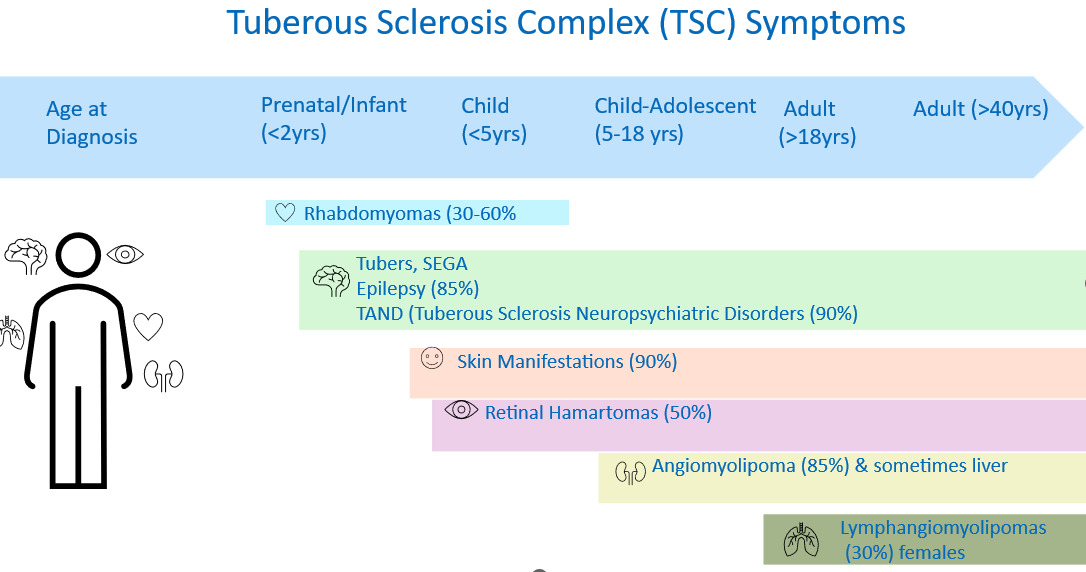
Tuberous Sclerosis Complex symptom emergence and progression Adapted from Northrup et al., 2021
Are the tumours cancerous?
No. The tumors resulting from TSC are not cancerous, but may still cause serious problems.
The tumours in the brain can cause epilepsy and seizures, as well as TSC- Associated Neuropsychiatric Disorders (TAND) which include behavioural, intellectual, academic, psycological, psychiatric and neuropsychological difficulties. They can also cause disruption to the flow of cerebrospinal fluid (CS F) making a child seriously ill.
The tumors in the kidney (renal angiomyolipomas) can bleed, causing haemmhorage which can be life threatening. They can also disrupt normal kidney function.
Heart tumors, called cardiac rhabdomyomas, can cause problems if they are blocking the flow of blood or cause abnormal heart rythms (arrhythmia).
Lung tumours lymphangioleimyomatosis (LAM) primarily affecting women, lead to lung destruction and breathing issues.
What are the Diagnostic Criteria and Surveillance and Management Recommendations ?
TSC diagnostic criteria and surveillance and management recommendations, updated in 2021 by a consortium of global TSC experts, provide a framework for optimal care of those living with TSC and their families.
Diagnostic Criteria
Definite TSC: Definite diagnosis of Tuberous Sclerosis Complex (TSC) requires either identifying a pathogenic varient in TSC1 or TSC 2 genes, or finding 2 major clinical features with 2 minor features.
Possible TSC: Either one major feature or > 2 minor features.**A combination of the two major clinical features LAM and angiomyolipomas without other features does not meet criteria for a Definite Diagnosis.

Surveillance and Management Recommendations
Individuals with a diagnosis of TSC require lifelong surveillance. At the time of diagnosis, many medical tests are performed and international consensus recommendations determine ongoing monitoring surveillance protocols. The following tables show surveillance screening for TSC according to the International Consensus recommendations Click here.
Medication Information
There are several types of medication used in the treatment of Tuberous Sclerosis and new medications are continuously being discovered and used. It is important to stay updated and obtain accurate information form reliable sources.
Medicines.ie, is Ireland’s central, regulator approved online resource of accurate information on medicines available in the Republic of Ireland. It provides information for healthcare professionals and the public through Summary of Product Characteristics (SPCs), Patient Information Leaflets (PILs) and Educational Materials. It is owned by the Irish Pharmaceutical Healhcare Association (IPHA) and designed for easy searching and accessing crutiol drug details https://www.medicines.ie/
Where can I find more information about TSC?
There are excellent websites hosted by TSC organisations worldwide where you will find extensive and comprehenssive information, resources and direction. We highly recommend you consult them.
TSCAlliance https://www.tscalliance.org/
Tuberous Sclerosis Association UK (TSA UK) https://tuberous-sclerosis.org/
Tuberous Sclerosis Australia https://tsa.org.au/
Tuberous Sclerosis International (TSCi) https://www.tscinternational.org/
Glossary
A
ADHD (Attention Deficit Hyperactivity Disorder)
A neurodevelopmental condition affecting attention, impulse control, and activity levels. ADHD is highly prevalent in individuals with TSC (30–50%) and forms part of TAND. It may co-exist with epilepsy and intellectual disability, requiring careful management of medications.
🔗 https://adhdireland.ie/general-information/what-is-adhd/
🔗 https://tandconsortium.org/about/
AML (Angiomyolipoma)
A benign tumour made up of blood vessels, smooth muscle, and fat, most commonly affecting the kidneys in TSC (70–80% of patients). AMLs can grow and bleed, requiring monitoring or treatment (e.g. mTOR inhibitors or embolisation).
🔗 https://www.kidneycareuk.org/about-kidney-health/conditions/angiomyolipoma/
ASD (Autism Spectrum Disorder)
A neurodevelopmental condition affecting communication, behaviour, and social interaction. Up to 69% of individuals with TSC may meet criteria for ASD. Early diagnosis improves outcomes.
🔗 https://tandconsortium.org/
Autosomal Dominant
A genetic inheritance pattern where only one altered copy of a gene (TSC1 or TSC2) is required to cause TSC. Each child of an affected parent has a 50% chance of inheriting the condition.
🔗 https://medlineplus.gov/genetics/understanding/inheritance/inheritancepatterns/
Autosomal (General)
Refers to genes located on non-sex chromosomes, meaning the condition affects males and females equally.
🔗 https://www.genome.gov/genetics-glossary/Autosomal-Dominant-Disorder
B
Benign Tumour
A non-cancerous growth that does not spread but may still cause problems depending on location. In TSC, benign tumours can occur in multiple organs including brain, kidneys, heart, lungs, and skin.
🔗 https://www.nhs.uk/conditions/benign-brain-tumour/
C
Cardiac Rhabdomyoma (cRHM)
A benign tumour of the heart, often detected during pregnancy or infancy. It is one of the earliest indicators of TSC and often regresses naturally over time.
🔗 https://www.tscalliance.org/understanding-tsc/associated-disorders/#cardiac
Cortical Tuber
A disorganised area of brain tissue found in the cerebral cortex. These lesions are strongly associated with epilepsy, developmental delay, and cognitive differences in TSC.
🔗 https://www.epilepsy.com/what-is-epilepsy/related-conditions/tuberous-sclerosis-complex
CT (Computed Tomography)
A type of imaging scan that uses X-rays to create detailed cross-sectional images of the body. Used in TSC surveillance when MRI is not suitable.
🔗 https://www.hse.ie/eng/health/az/c/computed-tomography-ct-scan/
D
Dental Enamel Pits
Small defects in the enamel of teeth commonly seen in individuals with TSC. They are usually harmless but can assist in diagnosis.
🔗 https://www.tscalliance.org/understanding-tsc/associated-disorders/#dental
De Novo Mutation (Sporadic Mutation)
A new genetic mutation occurring for the first time in a child, without being inherited from either parent. Around two-thirds of TSC cases arise this way.
🔗 https://medlineplus.gov/genetics/understanding/mutationsanddisorders/
E
EEG (Electroencephalogram)
A test that measures electrical activity in the brain and is used to diagnose and monitor epilepsy in TSC.
🔗 https://www.epilepsy.ie/content/eeg
Epilepsy
A neurological condition characterised by recurrent seizures. It affects up to 90% of individuals with TSC and is often one of the earliest clinical features.
🔗 https://www.epilepsy.ie/content/tuberous-sclerosis-complex
Everolimus (mTOR Inhibitor)
A targeted therapy used to treat TSC-related tumours (e.g. SEGA, AML) and sometimes epilepsy by inhibiting the mTOR pathway.
🔗 https://www.ema.europa.eu/en/medicines/human/EPAR/votubia
H
Hamartoma
A benign, tumour-like growth made up of disorganised but normal tissue elements. TSC is characterised by widespread hamartomas.
🔗 https://rarediseases.org/rare-diseases/tuberous-sclerosis/
Hamartin–Tuberin Complex
Proteins produced by the TSC1 and TSC2 genes that regulate cell growth via the mTOR pathway. Dysfunction leads to uncontrolled growth and tumour formation.
🔗 https://www.nature.com/subjects/mtor-signaling
Hydrocephalus
A build-up of cerebrospinal fluid in the brain, often caused by a SEGA blocking fluid pathways, requiring urgent treatment.
🔗 https://www.nhs.uk/conditions/hydrocephalus/
I
Infantile Spasms (IS)
A severe form of epilepsy occurring in infancy, commonly associated with TSC. Early treatment (often with vigabatrin) is critical.
🔗 https://www.epilepsy.ie/content/infantile-spasms
Intellectual Disability (ID)
A condition involving limitations in intellectual functioning and adaptive behaviour. It can range from mild to severe in TSC.
🔗 https://www.hse.ie/eng/services/list/4/disability/
L
LAM (Lymphangioleiomyomatosis)
A progressive lung disease affecting mainly women with TSC, caused by abnormal smooth muscle cell growth in the lungs.
🔗 https://www.europeanlung.org/en/information-hub/lung-conditions/lymphangioleiomyomatosis/
M
MRI (Magnetic Resonance Imaging)
A detailed imaging technique using magnetic fields to visualise internal organs, particularly important for brain and kidney monitoring in TSC.
🔗 https://www.hse.ie/eng/health/az/m/mri-scan/
mTOR Pathway
A cellular signalling pathway that regulates growth and metabolism. Overactivation due to TSC mutations leads to tumour formation.
🔗 https://www.nature.com/subjects/mtor-signaling
mTOR Inhibitors (Rapalogs)
Medications such as everolimus and sirolimus that suppress abnormal cell growth in TSC by targeting the mTOR pathway.
Multidisciplinary Team (MDT)
A coordinated group of specialists (neurology, nephrology, dermatology, psychiatry, etc.) providing comprehensive TSC care.
🔗 https://www.hse.ie/eng/about/who/cspd/ncps/mdt/
P
Phakomatosis
A group of genetic disorders (including TSC) characterised by abnormalities in the skin, brain, and eyes.
🔗 https://www.ncbi.nlm.nih.gov/books/NBK560728/
R
Retinal Hamartoma (Phakoma)
A benign tumour on the retina that may affect vision but is often asymptomatic.
🔗 https://www.aao.org/eye-health/diseases/retinal-hamartoma
Renal (Kidney-related)
Refers to the kidneys. Renal complications such as AML are a major concern in TSC.
🔗 https://www.hse.ie/eng/health/az/k/kidney-disease/
S
SEGA (Subependymal Giant Cell Astrocytoma)
A slow-growing brain tumour that can block cerebrospinal fluid flow and cause hydrocephalus. Requires monitoring and sometimes surgery or medication.
🔗 https://www.tscalliance.org/understanding-tsc/associated-disorders/#sega
SEN (Subependymal Nodule)
Small benign growths along the brain ventricles that may develop into SEGA.
Seizure
A sudden burst of abnormal electrical activity in the brain. Seizure types vary widely in TSC.
🔗 https://www.epilepsy.ie/content/seizures
Shagreen Patch
A thickened, leathery patch of skin, typically found on the lower back. A classic dermatological sign of TSC.
Surveillance
Lifelong monitoring using imaging and clinical review to detect complications early and guide treatment.
🔗 https://www.tscalliance.org/resources/tsc-diagnostic-criteria-surveillance-and-management-guidelines/
T
TAND (TSC-Associated Neuropsychiatric Disorders)
An umbrella term covering cognitive, behavioural, psychiatric, academic, and psychosocial difficulties experienced by up to 90% of individuals with TSC.
🔗 https://tandconsortium.org/
TSC (Tuberous Sclerosis Complex)
A rare, multisystem genetic condition caused by mutations in TSC1 or TSC2, leading to benign tumours in multiple organs.
🔗 https://www.orpha.net/en/disease/detail/805
TSC1 Gene
Located on chromosome 9, this gene produces hamartin, a protein that regulates cell growth.
TSC2 Gene
Located on chromosome 16, this gene produces tuberin, which works with hamartin to suppress tumour formation.
U
Ungual Fibroma (Koenen’s Tumour)
Small benign growths around or under fingernails or toenails, often appearing in adolescence or adulthood.
V
Variable Expressivity
The degree to which TSC symptoms vary between individuals, even within the same family.
Vigabatrin
A first-line anti-seizure medication used particularly for infantile spasms in TSC.
🔗 https://www.hpra.ie/homepage/medicines
Clinical & Medical
EEG – Electroencephalogram
MRI – Magnetic Resonance Imaging
CT – Computed Tomography
AML – Angiomyolipoma
SEGA – Subependymal Giant Cell Astrocytoma
SEN – Subependymal Nodule
LAM – Lymphangioleiomyomatosis
TSC-Specific
TSC – Tuberous Sclerosis Complex
TAND – TSC-Associated Neuropsychiatric Disorders
TAND-L / TAND-SQ – TAND tools
Irish Healthcare Context
HSE – Health Service Executive
GP – General Practitioner
CAMHS – Child & Adolescent Mental Health Services
Research & Policy
ERN – European Reference Networks
IRDiRC – International Rare Disease Research Consortium
HRB – Health Research Board

